The Impact of COVID-19 on Maternal Health Services: A Qualitative Study on Midwives in Cox’s Bazar, Bangladesh
Ashley Pugh, Arman Mahmood, Johanna Hansing, Iftikher Mahmood
All authors associated with HOPE Foundation for Women and Children of Bangladesh
Corresponding Authors: Iftikher Mahmood
Correspondence: E-mail: iumahmood@gmail.com
Introduction
In 2020 the world was shocked by the development and exacerbated spread of COVID-19 that has rendered economies weak, dissipated health systems, and revealed gross inequities. It has demonstrated weaknesses within our health sectors, amongst our populations, and above all, made us acutely aware that we are all susceptible and atrisk. COVID-19 will alter our behaviors and processes in almost every single sector and do so for the foreseeable future. We know that necessary measures such as lockdowns have crippled many economies at the macro-level, and at the micro-level, adversely impacted most families through job loss, the reduction of income generation opportunities, morbidity, and mortality. The United Nations estimates the pandemic will push the number of people living in extreme poverty to over one billion by 20301 . This study seeks to understand the impact COVID-19 has had on the maternal and child health sector in rural areas by understanding the impacts on practicing midwives, as well as the effect on the health-seeking behavior of their patients.
Maternal and Child Health in Low Resource Settings
Maternal and Child Health is a field of health that already brings challenges and vulnerabilities. In conjunction with COVID-19, and in lower developed regions, adverse outcomes are expected in both developed and less developed countries alike. Less developed countries, however, carry specific challenges that become more complicated with a pandemic. This occurrence has been studied related to past epidemics such as SARS and Ebola, and similar predictions are being drawn from this research and applied to COVID-19. In regards to maternal health and COVID-19 specifically, Nawsherwan et al. (2020) concluded that COVID-19 pneumonia in pregnant women could lead to complications such as premature birth, fetal distress, and NRDS2 . Moreover, while women of reproductive age and children are not the most at-risk groups, they are highly affected by disruptions in health services, the redirect of resources for COVID-19 efforts, and the closing of peripheral health centers3 . This was seen with the Ebola outbreak in West Africa4 . Similarly, during the Ebola outbreak, a 2014 study reports that antenatal care coverage decreased 22 percentage points, family planning decreased by 6 points, facility-based delivery 8 points, and postnatal care 13 points5 . Qualitative findings pointed to a fear of contracting the Ebola virus, mistrust of the health systems, and misunderstanding about the disease origination as reasons for the decrease in utilization6 . During the SARS outbreak, ambulatory care decreased 23.9% in Taiwan and in-patient care by 35.2%7
COVID-19 has halted RMNCH campaigns and services such as vaccinations, mosquito nets, and Vitamin A supplementation8 , and further disrupted pharmaceutical and supply chains. This is made worse for lower developed countries who have less buying power9 . Necessary maternal and child health supplies and medication can be scarce in areas where all resources have been allocated to purchasing the same effects but to battle COVID-19. This inequity has already been witnessed considering that wealthy countries have bought half of the projected COVID-19 vaccines10. Moreover, mobility and public transportation restrictions are likely to further reduce access to maternal and child health facilities and services, coupled with economic burden that puts the transportation and cost for these services out of reach for those impoverished. Additionally, the disruption to transport and supply chains will likely result in food shortages, and families bearing financial losses related to the pandemic will have difficulty purchasing nutritious foods, elevating the risk for malnutrition in the family. Lastly, Busch-Hallen et al. concluded that breastfeeding practices are impacted by COVID-19 as there is a reduction of ANC and PNC visits, health care providers are discouraging breastfeeding due to fear of mother to infant transmission, and home environments that once enabled breastfeeding are no longer enabling as lockdowns place additional pressure on women to provide child care and educational supports to older children11. Bearing all of the above in mind and given that these are unprecedented times, Roberton et al. used modelling of three different scenarios to predict the impact on maternal and child health in low-income countries. Their results state that:
“…if the COVID-19 pandemic results in widespread disruption to health systems and reduced access to food, LMICs can expect to see large increases in maternal and child deaths. Under our first scenario (coverage reductions of 9·8–18·5% and wasting increase of 10%), over 6 months there would be 253,500 additional child deaths and 12,200 additional maternal deaths. Under our third scenario (coverage reductions of 39·3–51·9% and wasting increase of 50%), over 6 months there would be 1,157,000 additional child deaths and 56,700 additional maternal deaths. These deaths would represent a 9.8–44.7% increase in under-5 child deaths per month, and an 8.3–38.6% increase in maternal deaths per month, across the 118 countries12.”
Midwifery
Midwifery is considered a best buy in improving maternal and child health outcomes. Midwifery is defined as “the health services and health workforce needed to support and care for women and newborns, including sexual and reproductive health and especially pregnancy, labour and postnatal care.” (UNFPA). This profession has been largely neglected in recent times, mostly due to the overmedicalization of pregnancy care and a lack of resources for recruiting and retaining midwives. When trained and educated to internationally accepted standards, midwives have the competencies to deliver 87% of essential services for women and newborns. Not only are they fully competent to care for women and their newborns, but they can do so at a much lower price point. In the United States, one of the most costly countries to deliver in, women who need delivery by C-section pay on average $15,000 USD while natural delivery costs approximately $11,200 USD. In South Africa, delivering naturally costs about $2,000 USD despite only a marginal proportion of the population having the money to afford that, due to inequities and a lack of health insurance. UNICEF has reported that nearly five million families living in Africa, Asia, Latin America, and the Caribbean spend upwards of 40% of their annual household expenses on maternal health13. The work midwives do is comprehensive, ranging from essential pre and post care, provide contraceptive advice as well as education and counseling on breastfeeding, examining for noncommunicable diseases during antenatal care checks such as blood pressure and blood sugar, screening for malaria, tuberculosis, HIV and other STIs, screening for breast and cervical cancer and acting as watchdogs in the community and advocates for the women they serve. The UNFPA calculated that investing in midwifery education coupled with deployment to community-based posts can yield a 16- fold return on investment in terms of lives saved and the cost savings in reducing expenditure on cesarean sections. Therefore, the UNFPA considers midwives a best buy
The Study
This study took place in the district of Cox’s Bazar, Bangladesh, a population of 2,988,47314. Cox’s Bazar is located in southeast Bangladesh, neighboring Myanmar. At present, Cox’s Bazar is home to the largest refugee camp, hosting an estimated one million Rohingya refugees who escaped violence and persecution in Myanmar. The Joint Response Plan15 identified that of those refugees living in the camps, 52% are female, of which 23% are between the ages of 18 and 5916. A total of 474,014 women and girls currently live in the camps, and approximately 22,000 were pregnant as of January 201917. The presence of refugee camps poses a significantly increased risk for COVID-19 infection and spread due to the close living proximities of the refugees, poor health amongst refugees in need of care, and the lack of resources for infection prevention. Furthermore, the Cox’s Bazar district is made up of many rural areas, which makes accessing health care for its population challenging. This is particularly true for maternal health; in rural areas of Cox’s Bazar it is estimated that 9 out of 10 women give birth at home, often at the hands of untrained attendants18. The conservative, rural areas often lack awareness and understanding of the needs of pregnant women, which often clash with cultural values; they lack the financial capacity to pay for maternal health services and transportation to the services and are often deterred from receiving services due to past negative experiences at health facilities, coupled with lack of access. These barriers are presumed to be exacerbated by COVID-19.
HOPE Maternity Care Facilities
HOPE Foundation for Women and Children of Bangladesh is a non-profit organization that has served the area of Cox’s Bazar since 1999. HOPE Foundation’s goal is to improve maternal and child health, and has become a pioneer in southeastern Bangladesh through its work in fistula treatment and prevention and the training and deployment of midwives. HOPE trains midwives annually through the Three-Year Community-based Midwifery Diploma Programme supported by the UK Department for International Development’s funding and with BRAC University’s academic and technical support. In an effort to retain these trained midwives to serve where they are needed most, HOPE established 13 HOPE Birth Centers. These centers are staffed by trained midwives in remote areas to increase access to maternal healthcare. The centers offer a referral system for at-risk pregnancies, a safe birthing haven, and a community-level approach to breaking down cultural barriers of seeking assistance from a professionallytrained healthcare provider. HOPE runs multiple hospitals in the area providing maternity and COVID care with a total in-patient bed capacity of 140 beds. Additionally, HOPE runs nine Sexual and Reproductive Health centers. All of HOPE’s facilities operate 24/7, with midwives serving as frontline providers for maternity and delivery services. In an effort to answer critical research questions on the impact of COVID-19 on maternal health, HOPE aimed to survey the midwives within its network.
Midwifery Survey
The survey was developed by the HOPE team and distributed to 50 practicing midwives. HOPE Foundation received a total of 27 completed surveys. Of the midwives surveyed, 74% have been a midwife for five years or less and 26% report being a midwife for one year or less. A total of 44% of these midwives work in a hospital setting, 22% in a sexual and reproductive health center, and 34% in a birth center. Of their described teams, 78% claim that they have a team of 5 or more that support them in their roles, while 22% report less than 5.
Results
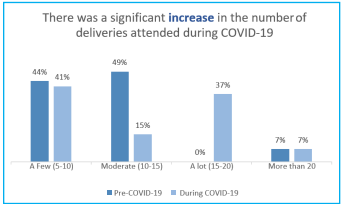
In comparing demand for services pre-COVID-19 to the present day, the midwives reported an overall increase in the number of deliveries they are performing each month, on average. There was a 0% change in those who delivered more than 20 babies a month, a 100% increase in those who reported delivering 15-20 babies per month, a 69% increase in those who delivered 10-15 a month, and an 8% decrease of those who reported only delivering 5-10 babies, present day under the conditions of COVID-19.
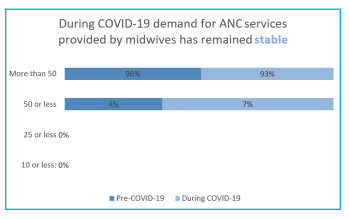
Regarding how many women they are referring to for Cesarean Section each month, that number has decreased during COVID-19. Prior to COVID-19, 63% reported five or less and 37% ten or less, respectively; present-day under COVID-19, 100% of midwives report referring five or less on average, each month. In terms of how many women they provided antenatal care to each month on average, PreCOVID saw the majority (96%) serve more than 50 women each month; post-onset of COVID-19, the demand remains stable with the majority (93%) providing ANC to 50 women or more and 7% providing services to 50 women or less.
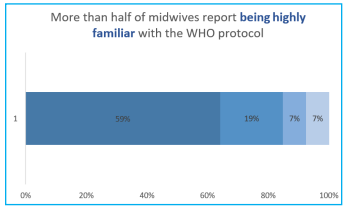
In an effort to understand a potential difference in clinical presentations, the survey asked midwives which maternal complications they witness, both pre- and post-onset of COVID-19. There was not any statistically significant difference in the presenting conditions. The conditions that saw an increase post- onset of COVID-19 were postpartum hemorrhage (5% increase), obstructed labor (10% increase), and diabetes (33% increase). The following conditions saw a decrease: Pre-eclampsia (7%), high blood pressure (16%), infection (25%). A total of 63% of midwives report seeing more complications in their patients since the start of COVID-19, 22% feel as though there is no change, and 11% report seeing less. The survey then pivoted to asking questions specifically about COVID-19 to better understand the conditions the midwives are working in, as well as their attitudes towards the work. On a scale of 0 to 10 (0 being not familiar and 10 being highly familiar), when asked about how familiar the midwives are with the WHO protocol, 59% report being highly familiar, 19% very familiar, 7% familiar, In an effort to understand a potential difference in clinical presentations, the survey asked midwives which maternal complications they witness, both pre- and post-onset of COVID-19. There was not any statistically significant difference in the presenting conditions. The conditions that saw an increase post- onset of COVID-19 were postpartum hemorrhage (5% increase), obstructed labor (10% increase), and diabetes (33% increase). The following conditions saw a decrease: Pre-eclampsia (7%), high blood pressure (16%), infection (25%). A total of 63% of midwives report seeing more complications in their patients since the start of COVID-19, 22% feel as though there is no change, and 11% report seeing less. The survey then pivoted to asking questions specifically about COVID-19 to better understand the conditions the midwives are working in, as well as their attitudes towards the work. On a scale of 0 to 10 (0 being not familiar and 10 being highly familiar), when asked about how familiar the midwives are with the WHO protocol, 59% report being highly familiar, 19% very familiar, 7% familiar,
59% of midwives reported receiving additional training during the time of COVID-19, while 41% have not. A total of 52% reported a shortage of health supplies during COVID-19 while 48% did not experience a shortage. It is important to note that those who experienced a shortage were operating out of clinics in remote areas; those working within hospitals did not report a shortage. Moreover, midwives answered that during antenatal care visits, they are utilizing the following PPE: disposable mask (89%), gloves (59%), homemade mask (56%), goggles (44%) and N95 mask (11%), respectively. During delivery the PPE used takes into consideration more caution and protection with disposable mask (89%), gloves (100%), homemade mask (19%), goggles (93%), and N95 masks (19%). For the staff who sanitize post-delivery, 56% utilize a mask, visor, and gown while 46% use just a mask and gown. All midwives stated that the community they serve received messaging on accessing maternal health care services during COVID-19. Only 19% of midwives report health facilities around them having closed due to the pandemic. In terms of the challenges that they have seen COVID-19 have on pregnant women, 7% of midwives reported families do not have money for healthcare, 7% report an increase in child marriages, 37% report an increase in adolescent pregnancy, 63% report an increase in domestic abuse and 89% of midwives state that women are afraid to go to health facilities. In analyzing midwives’ attitudes towards their jobs during the pandemic 100% of midwives report that they do not feel forced to work during COVID-19, 100% are happy to continue working and, likewise, all midwives report feeling comfortable operating and providing care during COVID-19. When asked about additional supports that the midwives would like to receive, 82% would like to see an improved referral network, 78% an improved transportation network, 52% would like to participate in webinars and 30% in in-person training. Lastly, when asked about their own health during COVID-19, 59% of midwives report having had COVID-19 or flu-like symptoms; out of those 59%, only 12% report getting a COVID test, but 100% report seeking care for their sickness.
Discussion
Based on the results, we can deduct that demand for maternal health care services provided by midwives in rural areas remains stable, with an increase in demand for different services, albeit many midwives with the perception that women are afraid to visit health facilities. This stresses the need to continue efforts by increasing messaging to women and communities about the safety of health facilities during times such as COVID-19 and the importance to not delay seeking care, particularly when pregnant or in labor. This messaging can be done through direct outreach to known pregnant women at their homes, mobile phones, and text messages. Additional work could be undertaken to understand the women’s preference in rural areas during the pandemic to visit a midwife who is not attached to a large health facility, versus seeking care at a hospital, for example. Moreover, given the familiarity with the WHO protocol and the utilization of PPE, midwives in rural Cox’s Bazar seem to have the necessary skills and equipment to continue operating during COVID-19; this is strengthened by their positive attitudes and commitment to continuing their work during the pandemic.
From this study, it is understood that there is a need for increased support for victims of and at-risk individuals of domestic abuse. Where possible, investment in additional social workers in both facilities for community outreach should be made. The same idea is relevant for preventing adolescent pregnancy and child marriage, which is likely to increase during a pandemic. Similarly, staff of facilities and outpatient centers should be equally trained in the above topics, when it is not possible to hire or recruit a social worker. In parallel, community workers can provide education on these topics to bring awareness and promote their prevention.
Moreover, given the stable demand for services, greater support should be lent to midwives operating in remote areas. These midwives are on the frontline working in fragile conditions, with scarce resources to both provide maternal health services and identify COVID-positive patients. Provided their leadership at this time in providing care to communities that are often isolated, they should be invited to the table when it comes to policy-making on COVID-19. Their experiences on-the-ground, and their thorough understanding of the community and its behaviors and perceptions makes them invaluable players. Equally so, given their request for better referral and transportation networks, greater partnerships should be forged amongst facilities - particularly during this challenging time. Investment into ambulatory services should be made so that COVID patients and non-COVID emergency patients can reach the point of care on time, preventing loss of life, and reducing morbidity. Lastly, expanded access to testing for midwives who are frontline health workers, particularly given their close contact to communities and especially pregnant women and newborns, is critical.
1. https://sdgintegration.undp.org/acceleratingdevelopment-progressduring-covid-19
2. https://link.springer.com/article/10.1007/s12098-020- 03372-2
3. https://www.thelancet.com/journals/langlo/article/ PIIS2214-109X(20)30229-1/fulltext
4. Brolin Ribacke KJ Saulnier DD Eriksson A von Schreeb J. Effects of the west Africa Ebola virus disease on health care utilization—a systematic review. Front Public Health. 2016; 4: 222
5. Counting indirect crisis-related deaths in the context of a low-resilience health system: the case of maternal and neonatal health during the Ebola epidemic in Sierra Leone. Health Policy Plan. 2017; 32: 32-39
6. Elston JWT Moosa AJ Moses F et al. Impact of the Ebola outbreak on health systems and population health in Sierra Leone. J Public Health (Oxf). 2016; 38: 673-678
7. Rust G Melbourne M Truman BI Daniels E Fry-Johnson Y Curtin T Role of the primary care safety net in pandemic influenza. Am J Public Health. 2009; 99: S316-S323
8. WHO Guiding principles for immunization activities during the COVID-19 pandemic. Interim guidance.https:// apps.who.int/iris/bitstream/handle/10665/331590/WHO2019-nCoV-immunization_services-2020.1- eng.pdf Date: March 26, 2020
9. WHO COVID-19. Situation update for the WHO African Region, 18 March 2020: external situation report 3. https:// apps.who.int/iris/bitstream/handle/10665/331487/SITREP_ COVID-19_WHOAFRO_20200318-eng.pdf
10. https://www.economist.com/graphic-detail/2020/11/12/ rich-countries-grab-half-of-projected-covid-19-vaccinesupply
11.https://www.thelancet.com/journals/langlo/article/PIIS2214-109X(20)30327-2/fulltext
12.https://www.thelancet.com/journals/langlo/article/PIIS2214-109X(20)30229-1/fulltext
13. https://news.un.org/en/story/2019/06/1039671
14. http://population.city/bangladesh/cox-s-bazaí/
15. https://íeliefweb.int/íepoít/bangladesh/2020-jointíesponse-plan-íohingya-humanitaíian-cíisis-januaíydecembeí-2020
16. BANGLADESH REFUGEE EMERGENCY: Population fact sheet [Internet]. Data2.unhcr.org. 2019 [cited
17 September 2019]. Available from: https://data2. unhcr.org/en/documents/download/70356
17. https://journals.plos.org/plosone/article?id=10.1371/ journal.pone.0230732
18. https://assets.publishing.seívice.gov.uk/media/ 57a08cf4ed915d622c0016a7/02-03_bangladesh.pdf